Applications
Neuraxial anesthesia is one of the most commonly provided forms of anesthesia in the US. Its use is seen frequently in obstetrics as well as orthopedics and various other specialties in the form of epidurals, spinals, or combined spinal-epidurals. These procedures are performed by directing a needle and/or catheter into the epidural or intrathecal space for directed administration of medications to block spinal nerves and is typically performed in the sitting position.
Although neuraxial anesthesia is considered the “gold-standard” for many of these procedures, patients may elect general anesthesia due to anxiety involving the perceived risks or the procedure process. The most notable risk—particularly in obstetrics—is that of accidental dural puncture and the resulting headache. Fear and anxiety surrounding the procedure has been found to be a primary factor in patient’s avoidance of neuraxial anesthesia, despite the possibility of improved outcomes.4,5
In addition to neuraxial procedure applications the EpiHug is also useful for a number of procedures which involve the sitting position. The Epihug improves positioning for erector spinae plane blocks, thoracentesis, thoracic ultrasound, and trigger point injections to name a few. The EpiHug serves to provide optimal positioning, minimize patient movement, and maximize patient comfort.
Position and Anxiety
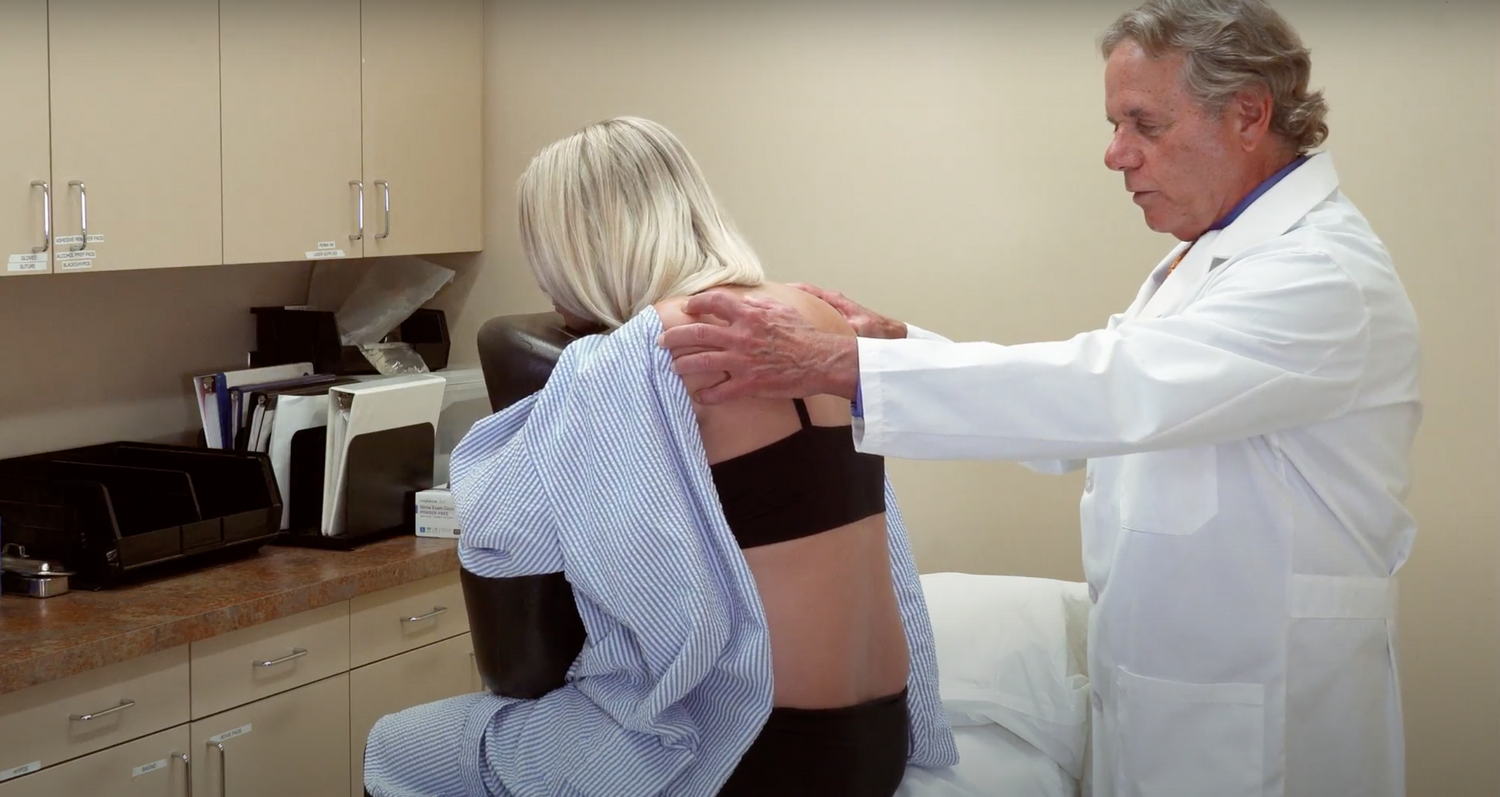
Proper positioning of the patient for neuraxial anesthesia is essential for a fast, successful nerve block. It has been shown to be an independent predictor for successful first attempt at neuraxial nerve block.1 In addition, a study in 2016 found patient movement and multiple epidural attempts to be among the most significant predictors for accidental dural puncture.2
The EpiHug is a device that addresses both the positioning and anxiety challenges surrounding neuraxial anesthesia. Optimum positioning is to remain straight without any lateral tilt, shoulders dropped, and head bent slightly forward to attain maximum flexion of the lumbar spine while keeping the lumbar spine perpendicular to the bed. Attaining maximum lumbar spinal flexion will allow the interspinous spaces to be more open and facilitate passage of a needle into the spinal or epidural space. Maintaining correct alignment is also of importance to minimize needle passes, particularly in cases where anatomic landmarks are less visible. The EpiHug provides a template for patients to easily attain the correct position and provides stability to reduce torsional, lateral, and anterior movement of the patient.
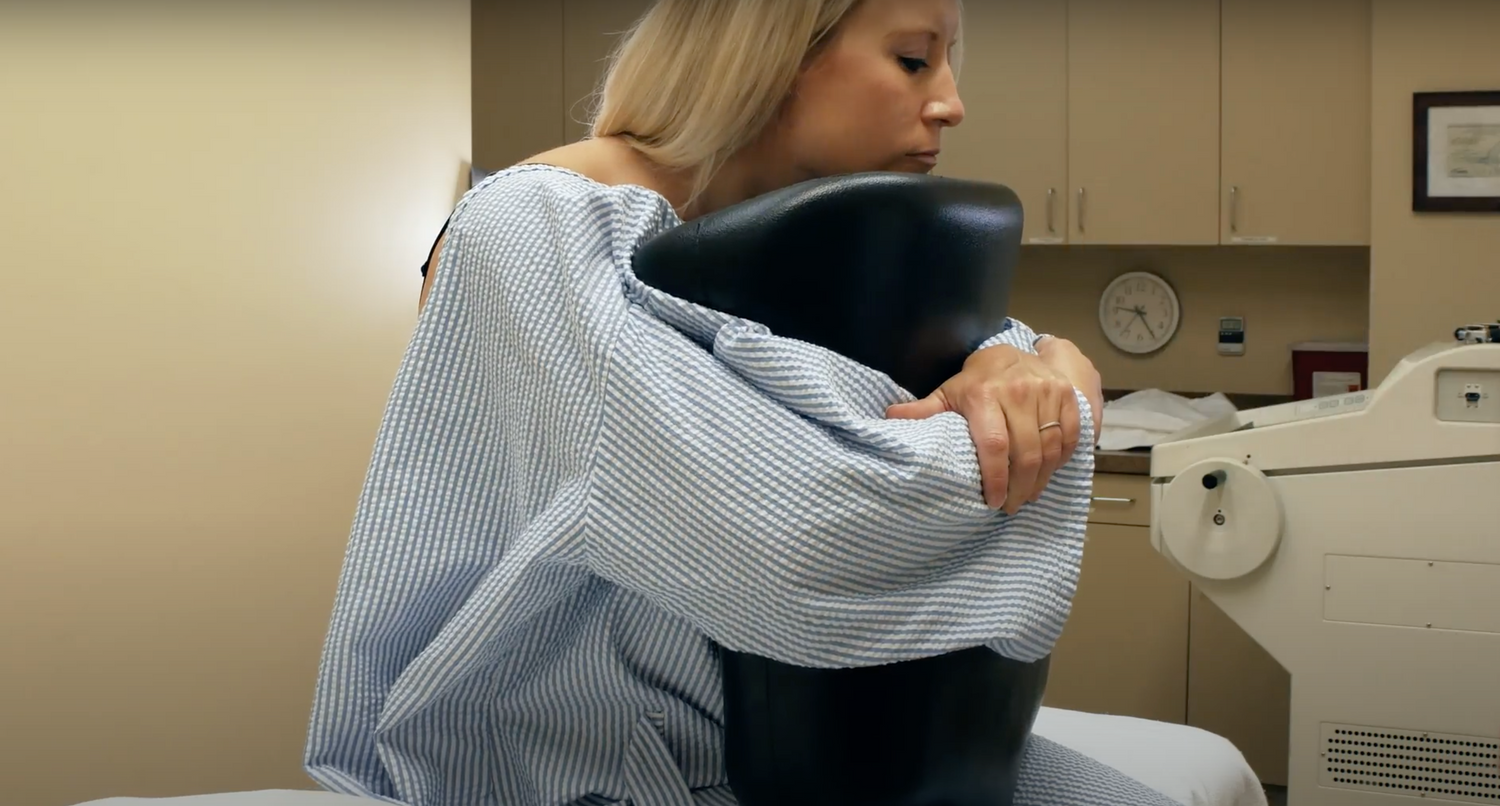
Proper Hug
In addition to facilitation of proper positioning, the foam maintains a density that allows for adequate support but is soft enough to allow for the patient to squeeze or “hug” the device and serve as a distraction technique for the patient while undergoing the procedure with the goal to decrease pain and anxiety. It has been effectively demonstrated that distraction techniques are useful in this regard for other needle-based procedures such as venipuncture.3

